Case Report co-authored by Dr Hannah Lock & Dr Marion Head, Ysbyty Gwynedd Emergency Department, North Wales, UK.
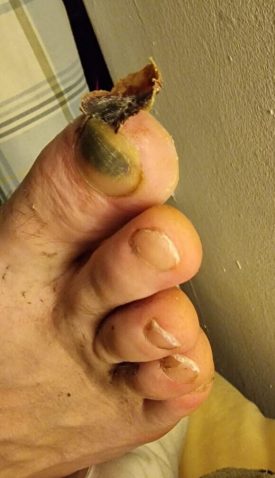
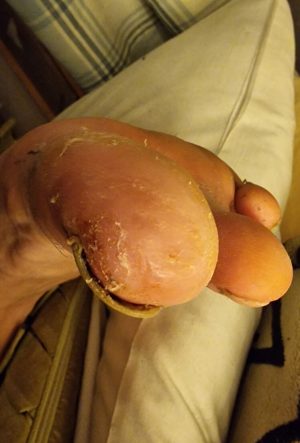
Last month, a young man walked into my emergency department with a simple but alarming complaint: “My toe has gone black.”
A week earlier, he had been camping on the glacier beneath the Aiguille du Midi in the Mont Blanc massif. Daytime temperatures were hovering around –22°C. After an uncomfortably cold first night camping, he and his partner decided to sleep in an unmanned mountain refuge on the second night, after a day mountaineering.
Later that evening, he walked back out across the glacier to collect equipment from their tent. During that short but bitterly cold journey, his big toe became painfully cold and then numb. By the time he returned to the refuge, the tip had turned pale. He attempted skin-to-skin rewarming, but the damage had already begun and the rewarming strategy wasn’t optimal.
A week later, back in the UK, the colour changes became more dramatic. By day 11, he presented to the emergency department for assessment.

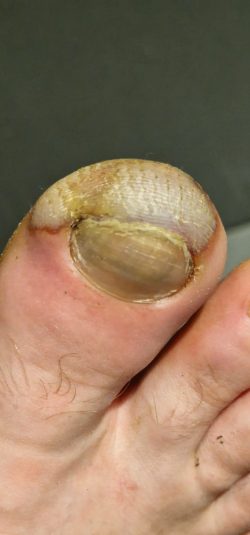
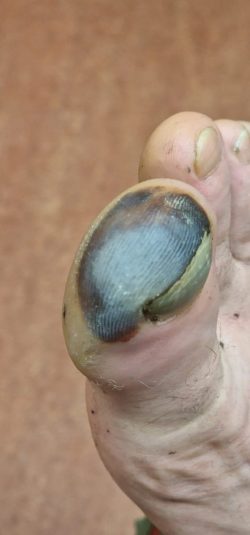
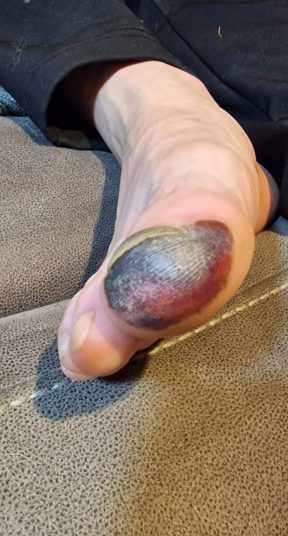
We diagnosed grade 1 frostbite. Given the timescale, he was outside the window for active vascular treatments to reduce the effects of his injury, so we managed him conservatively with ibuprofen, daily dressings with aloe vera cream, and orthopaedic follow-up.
Four weeks later, the necrotic tip of tissue separated and fell away, revealing healthy tissue beneath.
(Permission granted from the patient to use his story and images for educational purposes. Thank you!)
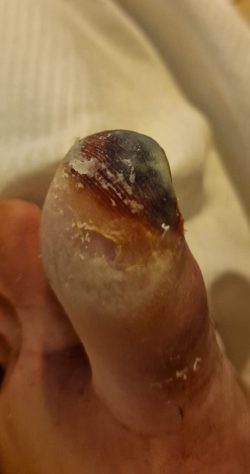
Understanding Frostbite:
What Is Frostbite?
Frostbite is the freezing of skin and deeper tissues. It is not simply “cold damage” — it is a complex injury involving both direct freezing and vascular compromise.
There are three key mechanisms:
1. Ice Crystal Formation
When tissue freezes, ice crystals form inside and outside cells, disrupting cellular structures and causing direct cell death.
2. Reduced Blood Flow
Cold exposure causes vasoconstriction. Small vessels narrow, blood flow slows, and tiny clots (microthrombosis) may form. The tissue becomes starved of oxygen.
3. Reperfusion Injury
Damage continues after thawing. As blood returns, inflammatory mediators worsen tissue injury.
Frostbite Evolution & Recognition
1. Early Signs
- Cold sensation
- Numbness
- White or pale skin
- Waxy appearance
- Hard or “woody” feel
2. After Rewarming
- Redness
- Swelling
- Bruising
- Blisters (clear or blood-filled)
3. Days to Weeks Later
- Black discolouration
- Dry, leathery eschar
- Necrosis
- Possible auto-amputation
Not everyone will develop all of these symptoms and signs, but these lists cover the general appearance that can be expected.
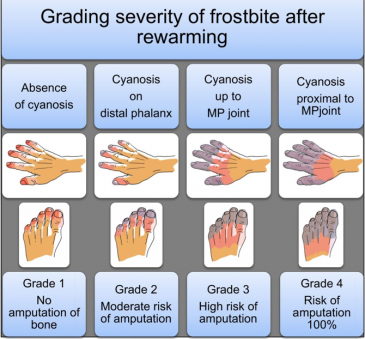
Grading Frostbite
Frostbite severity is commonly assessed using the Cauchy Classification, which helps predict the likelihood of tissue loss. This is based on the appearance of the affected area after rewarming.
Grading is important because it helps guide management decisions and prognosis.
In our patient’s case, the small necrotic tip that later detached without deeper tissue loss supports a grade 1 injury.
First Aid for Frostbite
Early management can dramatically alter outcomes.
Protect the Area
Do not walk on frostbitten feet. Prevent further cold exposure.
Only Rewarm if Refreezing Is Impossible
Refreezing causes devastating additional damage so if there is a chance your casualty’s limb may re-freeze, delay rewarming until you can protect from refreezing.
Rapid Rewarming
- Water bath at a temperature of 38–42°C (see photo below of what this might look like in practice in a mountain base camp setting)
- Duration: 30–60 minutes
- Keep water circulating
Pain Relief
Rewarming is painful — adequate analgesia is essential. Ibuprofen is particularly important, not just for pain but for its anti-inflammatory effects. Paracetamol and opioids may also be required.
Wound Care
- Air dry (do not rub)
- Apply aloe vera cream or gel (this has anti-inflammatory effects)
- Use sterile dressings
- Elevate to reduce swelling
- Clear blisters may be drained. Blood-filled blisters should be left intact
- Antibiotic if significant tissue loss


Hospital Management
Modern frostbite care has evolved significantly since the days of early surgery to amputate affected tissue and bone.
Delay Surgery
Early amputation is no longer recommended. Tissue that appears non-viable in the first days may recover. Delayed surgery preserves more tissue and bone.
Iloprost
For Grade 2–4 frostbite, intravenous Iloprost is now the drug of choice in experienced centres. Evidence since its introduction in frostbite treatment in 1994 shows improved limb salvage but only if used in the first few days following injury.
Iloprost:
- Dilates blood vessels
- Reduces platelet aggregation
- Improves microcirculation
- Reduces amputation rates
It’s important to note that not all hospitals have Iloprost available or clinicians with experience or knowledge of treating frostbite injuries. In these places, being advised to have early surgery by inexperienced clinicians may occur so it is vital that the casualty with frostbite is evacuated to a hospital with the relevant expertise and drug treatments.
Continue daily NSAIDs, aloe vera and dressings.

Preventing Frostbite Is Key
Frostbite is preventable — but only with preparation, vigilance, and good decision-making. Severe injuries often occur not because someone ignored the cold, but because they underestimated how quickly conditions can overwhelm exposed tissue.
Here’s how to reduce your risk.
Prepare For The Environment
Cold injuries occur when heat loss exceeds your body’s ability to maintain tissue temperature.
- Layer properly
- Stay dry
- Protect extremities and carry extra gloves
- Tight footwear reduces circulation — a major risk factor
- Keep moving and avoid prolonged immobility
- Eat and drink enough – cold environments increase metabolic demand
- Recognise and act on early warning signs – don’t ignore numbness!
- Carry a group shelter or other emergency kit
Frostbite risk increases with:
- Inexperience
- Temperatures below –10°C
- Wind exposure
- High altitude
- Night-time exposure
- Fatigue
- Poor nutrition and hydration
Higher risk groups include people with:
- Previous frostbite injury (increases susceptibility in the same area)
- Raynaud’s phenomenon
- Diabetes
- Peripheral vascular disease
- Smokers
- Children and elderly individuals
Travel With Knowledge
If travelling in extreme environments:
- Understand frostbite recognition and first aid
- Have a shelter plan
- Know evacuation routes and where the nearest, suitable hospital is with mountain medicine expertise
Final Thoughts
Frostbite is not just a mountaineering problem. It affects:
- Winter walkers
- Skiers
- Military personnel
- Homeless populations
- Outdoor workers and volunteers
Prevention depends on preparation, awareness, and timely decisions. In extreme cold, small choices make big differences.
If you spend time in cold, high-altitude or polar environments, understanding frostbite is not optional — it’s essential.
Our patient in this case was lucky not to have sustained a more severe frostbite injury.

Where to Get Advice
I’m working alongside a team of UK experts in frostbite care with the aim of improving outcomes for patients with frostbite injuries. We’re contactable 24/7 to offer advice to anyone who has a frostbite injury or is looking after someone who has one. Check out our website UK Frostbite Care. The site is currently undergoing improvements and will have lots more information available soon.
Another excellent website with lots of up to date, useful resources for clinicians and non-medical people is the Canadian Frostbite Care Network.
References:
Dallimore J., Anderson S. R., Imray C., Johnson C., Moore J. and Winser S. Oxford Handbook of Expedition and Wilderness Medicine. Third Edition. UK: Oxford University Press. 2023.
Scott E McIntosh, Luanne Freer, Colin K Grissom, George W Rodway, Gordon G Giesbrecht, Marion McDevitt, Christopher H Imray, Eric L Johnson, Prativa Pandey, Jennifer Dow, Peter H Hackett. Wilderness Medical Society Clinical Practice Guidelines for the Prevention and Treatment of Frostbite: 2024 Update. Wilderness Environ Med. June 2024; 35(2):183-197.
Charles Handford, Pauline Buxton, Katie Russell, Caitlin EA Imray, Scott E McIntosh, Luanne Freer, Amalia Cochran and Christopher HE Imray. Frostbite: a practical approach to hospital management. Extreme Physiology & Medicine. 2014, 3:7. http://www.extremephysiolmed.com/content/3/1/7
Marc-James Hallam, Tania Cubison, Baljit Dheansa, Chris Imray. Managing Frostbite. Clinical Review. BMJ | 27 November 2010 | Vol 341.
C Imray, A Grieve, S Dhillon and The Caudwell Xtreme Everest Research Group. Cold damage to the extremities: frostbite and non-freezing cold injuries. Postgrad. Med. J. 2009;85;481-488.
Alexander Poole, Josianne Gauthier, Mira MacLennan. Management of severe frostbite with iloprost, alteplase and heparin: a Yukon case series. 2021. CMAJ OPEN, 9(2).
Anne Kathrine Lorentzen, Christopher Davis, Luit Penninga. Interventions for frostbite injuries. Cochrane Database Syst Rev. Dec 20;2020(12).
https://ukfrostbite.com
https://frostbitecare.ca


What an excellent, simple and practical blog giving up to date advice. Thanks
Thanks Dave! I appreciate your positive comment and it’s great to hear you think the article is useful.